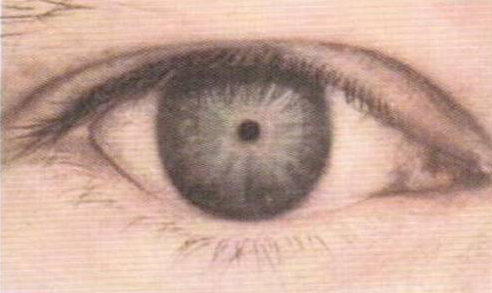
The cataract in the right eye eventually advanced, and the patient underwent uneventful phacoemulsification with a 5-mm dilated pupil 19 months after trabeculectomy. 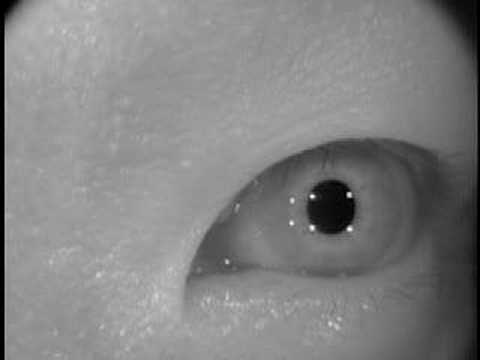
maintained an IOP of 8 mm Hg in this eye. Therapy con- sisting of one drop of bimatoprost q.h.s and one drop of dorzolamide b.i.d. He underwent a laser iridotomy on his left eye, which opened the angle to some degree, but it was difficult to asses because of the floating iris tissues blocking the view. There were no posttrabeculectomy complications in the patient's right eye, and his visual acuity improved to 20/50, with an IOP of 10 mm Hg. Peripheral iridectomy was also performed. He underwent a trabeculectomy alone in his right eye. He was eventually on maximally tolerated medical therapy in his right eye, but the IOPs remained uncontrolled. Would a laser iridotomy benefit the patient's left eye? How would an eye with iridoschisis respond to such a procedure?Īfter the examination, we prescribed acetazolamide 250 mg divided b.i.d.If you planned phacoemulsification on his right eye, whether combined with the trabeculectomy or alone at a later date, how difficult would the procedure be due to the iridoschisis? Would dilation be a problem? Would the iris strands get in the way?.If the IOP in the patient's right eye remains uncon- trolled despite maximum medical therapy, would you perform a combined surgical procedure (trabeculecto- my and phacoemulsification) or a trabeculectomy alone on that eye, since there is also an existing mild cataract?.Our working impression was of iridoschisis with angle- closure glaucoma (ACG) in both eyes, far advanced in the right and moderate in the left. The Octopus (Haag- Streit USA Inc., Mason, OH) revealed far-advanced glaucomatous visual field loss in his right eye and mod- erate glaucomatous visual field loss in his left eye (Figure 2). The irides had a convex configuration, and both eyes had 360o iridotrabecular apposition. His left eye had closed angles with 30o inferior peripheral anterior synechiae. “In 1922, Schmitt first reported iris splitting, but it was Loewenstein and Foster in 1945 who proposed the term iridoschisis after presenting the first histopathological study of this condition.”įour-mirror gonioscopy in the patient's right eye revealed closed angles with 60o inferior peripheral anterior synechiae and iris strands touching the cornea at the 5-o'clock position. The IOPs measured 53 mm Hg OD and 18 mm Hg OS with a Goldmann applanation tonometer. The cup-to-disc ratios were O.8 OD and 0.5 OS. There was a +1 cortical cataract in the patient's right eye, but the lens in his left eye was clear. There was iris atrophy with stromal detachments at the periphery of the iris at the 5- to 7-o'clock positions, and iris strands were visible floating in the anterior cham- bers of both eyes (Figure 1). The slit-lamp examination showed conjunctival conges- tion with a 4-mm, sluggishly reactive pupil in his right eye. On examination, the patient's visual acuity was 20/200 OD, improving with pinhole testing to 20/100, and 20/20 OS. Both iris lesions demon- strated transillumination. He had no history of eye surgery, eye trauma, or laser iridotomy, although both of his iri- des looked like they had undergone poorly performed inferior peripheral iridotomies. He instilled one drop of bimatoprost in his right eye every night. He had been diagnosed with glaucoma 6 months earlier after experi- encing episodes of sudden blurring and redness in his right eye. A 52-year-old man presented to the Veterans Memorial Medical Center Eye Department in Quezon City, Philippines, for a second opinion.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
